What is Gingival Inflammation?
Which Problems Can It Cause?
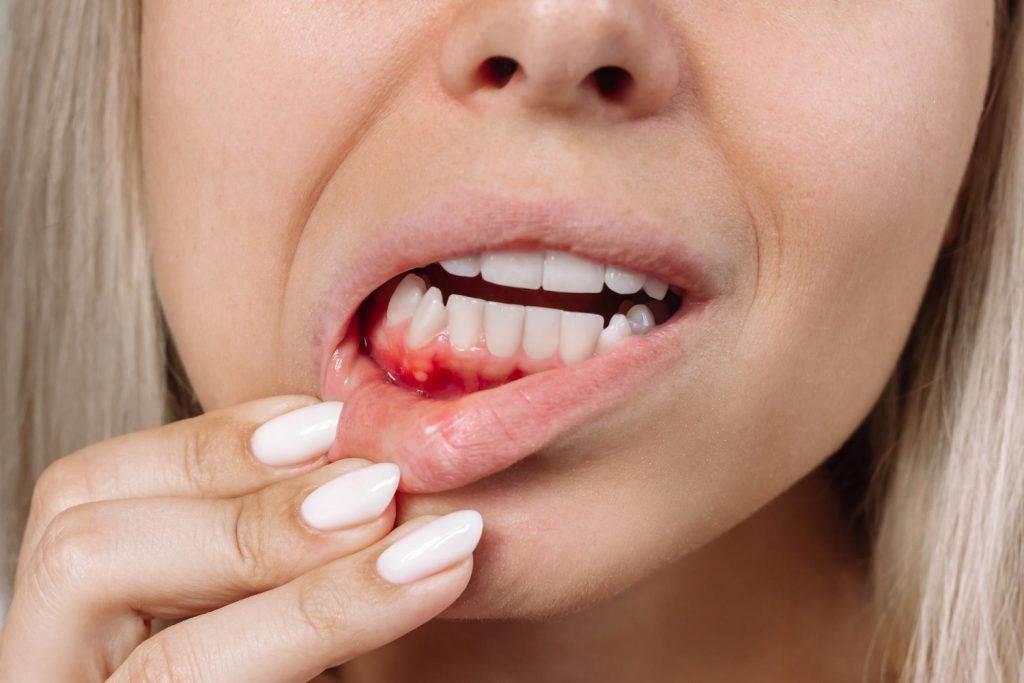
Gingivitis is an irritation and inflammation of the soft tissue surrounding the teeth caused by bacterial plaque and tartar. In the initial stage, mild symptoms such as redness, swelling and bleeding in the gums are seen. In the absence of proper oral care, the inflammation deepens and prepares the ground for gum recession and periodontal diseases. It is possible to maintain healthy gums with early diagnosis and intervention.
Contact Form
Get Detailed Information!
How Does Gingival Inflammation Occur?
Bacterial plaque that accumulates in the mouth sticks to the tooth surface over time, hardens and leads to tartar formation. Tartar irritates the gum line and causes inflammation. Poor brushing habits, lack of flossing, and neglecting regular dental check-ups accelerate the process.
Hormonal changes, certain medications and smoking can also trigger gingivitis.

How Can Gingival Inflammation Be Prevented?
Cleaning the teeth at least twice a day with regular and correct brushing is the first step in preventing plaque build-up. Using dental floss or an interdental brush to remove plaque between the teeth is also extremely important. Professional cleaning by a dentist every six months ensures the removal of tartar and treatment of problems detected at an early stage. A balanced diet and avoiding smoking provide additional protection.
What Happens If Gingival Inflammation Is Not Treated?
Untreated gingivitis can lead to the destruction of the connective tissue under the gum line and the jawbone. This process can progress to periodontal disease and tooth loss. In addition to tooth loss, chronic inflammation in the mouth can enter the systemic circulation and trigger general health problems such as heart disease and diabetes. Therefore, early intervention is vital.
What are the Symptoms of Gingival Inflammation?
Among the most common symptoms of gingivitis;
- Bleeding Gums
Bleeding when brushing or flossing is the earliest and most common sign of gingivitis. Healthy gums do not normally bleed; therefore, even a slight bleeding is a warning that requires intervention. - Red and Swollen Appearance
The gums, which should normally be pale pink in color, develop a dark pink-red hue and slight swelling. This change is a visual reflection of the gum’s inflammatory response to bacterial attack. - Gum Sensitivity and Pain
Sensitivity or pain when brushing, chewing hard food or even light touching of the gums is caused by inflammation in the tissue stimulating the nerve endings. - Bad breath (Halitosis)
Bacteria that accumulate in infected gum tissue produce foul-smelling volatile compounds. Constant or occasionally intense bad breath is one of the signs of gingivitis. - Gum recession
Progressive inflammation causes the gum tissue to move away from the tooth and the tooth root to be exposed. This creates both a long appearance and cold-hot sensitivity in the teeth. - Swaying Sensation in Teeth
When gingivitis becomes chronic and destroys bone tissue, the teeth cannot hold firmly in place. A feeling of shaking or displacement indicates advanced gingivitis. - Painful or Irritated Oral Tissues
Sometimes redness and tenderness can occur not only in the gums, but also in the tissues inside the mouth, such as the inside of the cheek or the corners of the tongue; this indicates the spread of localized inflammation.
What Happens If Gingival Inflammation Is Not Treated?
Untreated gingivitis can lead to the destruction of the connective tissue under the gum line and the jawbone. This process can progress to periodontal disease and tooth loss. In addition to tooth loss, chronic inflammation in the mouth can enter the systemic circulation and trigger general health problems such as heart disease and diabetes. Therefore, early intervention is vital.
Which Methods Can Gingival Inflammation Be Treated?
The first step in the treatment of gingivitis is a professional dental cleaning (scaling and root planing). Deep cleaning ensures that bacterial deposits are removed from the tooth surface and under the gums.
In advanced cases, local or systemic antibiotic treatment is used for support. Surgical methods and flap operations may be required in extreme tissue damage.
What are the Home Remedies for Gingival Inflammation?
Gargling with salt water at home is a natural way to relieve gingivitis. Also, mouthwashes containing chlorhexidine can help reduce bacteria in short-term use.
Choosing a soft-bristled toothbrush and toothpastes formulated for sensitivity helps protect sensitive tissues. Regular oral hygiene and healthy eating habits can also slow down the process at home.
What is the Relationship Between Gingival Inflammation and the Immune System?
A strong immune system supports defense against bacteria in the mouth, while weak immunity leads to exacerbation of gingivitis. Diseases that affect the immune system, such as diabetes and HIV, aggravate gum problems.
Stress and insufficient sleep also reduce the body’s ability to fight infections, increasing the risk of inflammation. Therefore, maintaining general health is also critical for oral health.

Frequently Asked Questions
You can take a look at the common questions asked by our patients and contact us for all other questions you are curious about.
Yes, gingivitis can increase the risk of heart disease by increasing the level of inflammation in the body. Research shows that periodontal disease can negatively affect vascular health
While gingivitis can occur at any age, it can also occur in children if tooth brushing habits are inadequate. Especially hormonal changes during puberty can increase this risk.
Gingivitis during pregnancy can increase the risk of complications such as pre-eclampsia and premature birth. Therefore, it is very important to take care of oral and dental health during pregnancy.
Yes, gingivitis can cause bacteria to build up in the mouth, leading to bad breath. This can also have a negative impact on social relationships.
Smoking damages the gums, increasing the risk of inflammation. Smoking can also hide the symptoms of gum disease, making diagnosis and treatment more difficult.
Yes, left untreated, gingivitis can become chronic and lead to gum recession and tooth loss. Long-term inflammation can also negatively affect general health.
The bacteria that cause gingivitis can be passed on through saliva. Therefore, hygiene rules such as sharing a toothbrush or cutlery should be observed.



